Topics
- Article
- COVID-19
- Respiratory Rate
Leveraging WHOOP Technology to Predict COVID-19 Risk
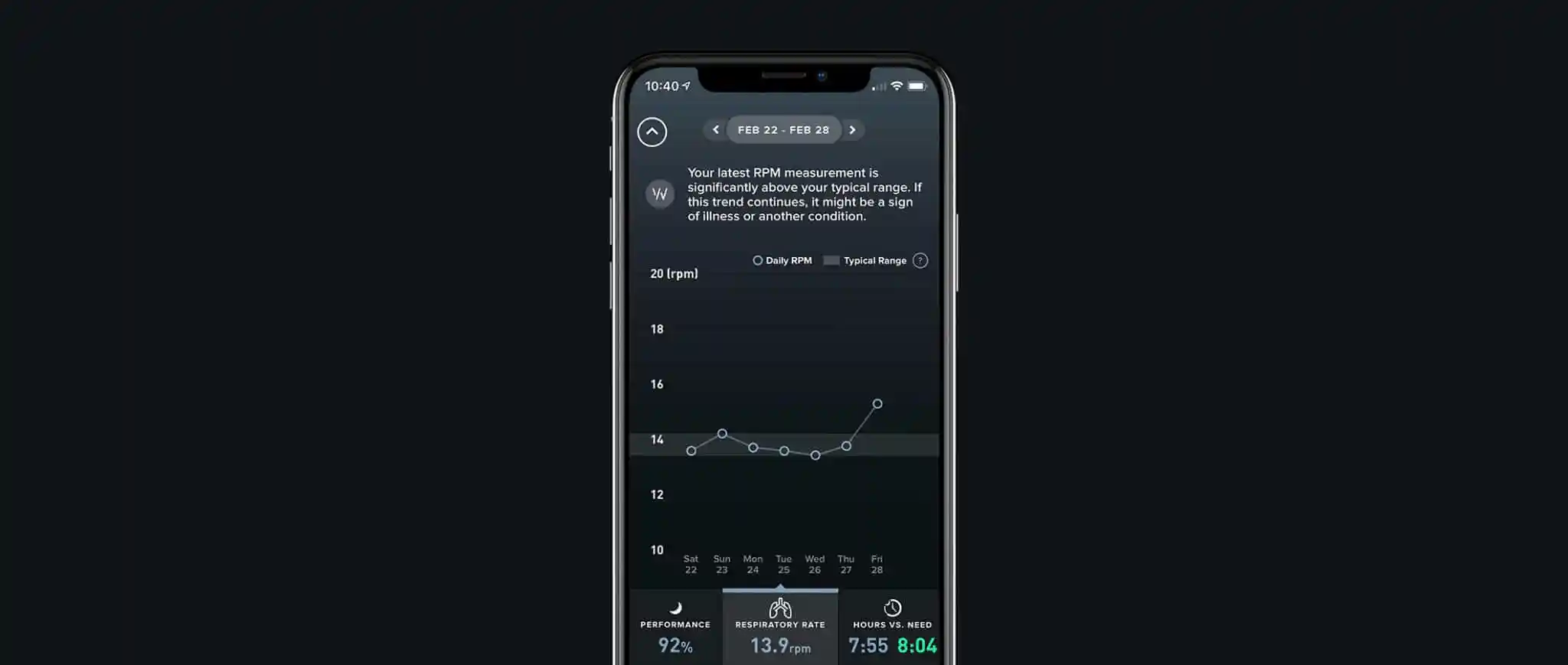
Study: Wearable Technology to Predict Risk of COVID-19 Using Respiratory Rate
UPDATE: Our paper Analyzing Changes in Respiratory Rate to Predict the Risk of COVID-19 Infection has been peer reviewed and published in the journal PLOS ONE. Read more below, originally posted June 22, 2020: Just over three months ago, I woke up to a message from a colleague showing me that one of our members had posted on social media about contracting COVID-19, and how his vital signs, as measured by WHOOP, had changed. One of the most dramatic differences we saw was in his respiratory rate. Not only did it jump an extraordinary amount, but his respiratory rate started rising during incubation before he realized he was sick. It became clear we needed to dig further into why that might be happening, so we enlisted our partners at Australia’s Central Queensland University to understand if this unusual observation was an anomaly or a useful early warning sign of COVID-19. WHOOP has submitted a manuscript for peer review and publication on the utility of wearable technology in providing early warning signs of potential COVID-19 infections. We believe this is a first-of-its kind submission for a maker of commercially available wearable technology. Over the past few months, WHOOP members have shared via our Journal feature their diagnoses of COVID-19, as well as many instances where suspected cases of COVID-19 resulted in negative tests. Using that data, we were able to derive an algorithm capable of identifying 80% of symptomatic COVID-19 cases simply from examining changes in respiratory rate from each member’s personal baseline.
Changes in Respiratory Rate As an Early Warning of COVID-19
The graph below shows the average percent change in respiratory rate from baseline by day relative to symptom onset (shaded in blue, notice the spike prior to this point). We found that in 20% of pre-symptomatic infected individuals, the rise in respiratory rate prior to symptom onset can be identified before they even know they are sick.
The average percent change in respiratory rate from baseline by day relative to symptom onset
Why is This Finding Important?
NON-INVASIVE, EARLY DETECTION
The finding that respiratory rate may deviate from baseline before we start to feel sick means it can potentially be leveraged to help keep others safe, by letting infected people know they might be capable of spreading COVID-19 so that they can socially distance. This is particularly exciting because WHOOP – which is to date the only wearable that has been validated by a third party clinical trial to accurately measure respiratory rate – can do so non-invasively and unobtrusively, by automatically taking measurements while you sleep each night, making monitoring this important vital sign extremely easy.
A SAFER RETURN TO WORK
This finding is particularly exciting because COVID-19 is actually most contagious in the 2 days before symptom onset. A common option many companies are exploring as they build out return-to-work strategies is to screen for fevers at the door and send home employees with elevated temperatures. Such an approach would likely be effective in removing some contagious employees from the workplace, but by definition is at the earliest catching people at symptom onset and therefore after contagiousness has already started to go down. On top of that, taking someone’s temperature at work means that they have already commuted into work and been in contact with colleagues and others, which increases the likelihood of spreading the virus.
Implications
WHOOP is not a medical product, and this study certainly doesn’t imply that those nasal swabs we’re in such short supply of are a thing of the past, rather it’s meant to demonstrate the power of continuous monitoring to leverage valuable information contained in subclinical changes in respiratory rate. “For the first time, we have shown that elevated respiratory rate, when compared to an individuals’ normal baseline, can be used to discriminate in some cases between people who test positive for COVID-19 and those who test negative," said Professor Greg Roach, Head of Sleep & Circadian Physiology Research, CQUniversity. Because medical screening of everyone every day is impractical, our study suggests that wearable-based solutions can serve as a useful tool to fill the gap between the ideal and reality, and give potentially infected individuals a valuable heads up that if heeded can prevent unnecessary continued community spread.
Going Forward
There is still more work to be done--the data we’ve been able to collect so far has been limited to symptomatic cases, so follow up research is required to understand if respiratory rate monitoring can aid in the detection of fully asymptomatic cases. Additionally, global shortages of testing limited the number of COVID-19 tested samples available for algorithm development and validation, as COVID-19 tests become more available WHOOP will continue to collect data and anticipates having access to more COVID-19 verified samples with which to refine this algorithm. At WHOOP, we’re committed to providing our members with scientifically sound research and a product that helps everyone continuously monitor themselves. As we work with leading universities and health organizations to investigate COVID-19 detection, symptoms, and recovery protocol, we will continue to update our technology to further enhance the WHOOP membership. Learn More: Why Your Respiratory Rate Matters — And How WHOOP Helps You Understand It The products and services of WHOOP are not medical devices, are not intended to diagnose COVID-19 or any other disease, and should not be used as a substitute for professional medical advice, diagnosis or treatment. All content available through the products and services of WHOOP is for general informational purposes only.