Topics
- Article
- Behavior Impact
- Organizations
Mind Manifested: How Psychedelics for Veterans with Depression and PTSD Impact WHOOP Data

In an effort to find solutions for the portion of the SFF veteran community who were not responding to traditional therapeutic interventions, SFF and WHOOP began exploring alternative methods to treat various mental illnesses.
The journey to unlock performance and support human thriving involves partnerships and research where we have the opportunity to explore how behaviors influence physiology and overall health. One of the primary objectives of our partnership with the SEAL Future Foundation (SFF), is to promote the wellness of the active duty and veteran SEAL community through various initiatives. This includes case studies and research that help us better understand the value of various treatment modalities within this unique population.
PTSD in Veteran SEALs
Post Traumatic Stress Disorder (PTSD) is a chronic illness, well-documented within the veteran population and is emerging as one of the most pressing public health issues due the COVID-19 pandemic and rising visibility of systemic oppression. The research emerging from Imperial College of London, MAPS, John Hopkins, Yale and others suggest that MDMA and psychedelic-assisted psychotherapies might be the breakthrough the world needs right now. In our work with SFF over years, it has become clear that there is a tremendous need to investigate new and novel medications to treat post traumatic stress disorder (PTSD), as well as the co-occurring mental illness, depression. PTSD is a leading cause of distress and disability among veterans and there are limited pharmacologic interventions. While two medications are currently FDA approved for PTSD, both antidepressants, the efficacy of these medications is quite limited. Some people do very well with them, but many others show little to no improvement in their symptoms. Further, these medications take weeks to months to reach their full benefit, and often even when some symptoms improve, others do not.
Psychedelics as an Alternative Treatment for PTSD
In an effort to find solutions for the portion of the SFF veteran community who were not responding to traditional therapeutic interventions, SFF and WHOOP began exploring alternative methods to treat various mental illnesses. We quickly learned about promising psychedelic research at Imperial College of London, led by the brilliant Dr. Robin Carhart-Harris, as well as other on-going work at the Multidisciplinary Association for Psychedelic Studies (MAPS), John Hopkins University, New York University and Yale, among others. According to Dr. William Richards, Psychologist and Research Affiliate at John Hopkins Center for Psychedelic and Consciousness Research, psychedelics, despite a few caveats, are “remarkably safe” for most people. They're not toxic or addictive, and they can be profoundly helpful. Richards continues to say that “psychedelics show ‘immense’ promise when it comes to treating mental health disorders.”
What Are Psychedelics Actually?
“Psychedelics”, in literal terms, mean “psyche” which is “mind,” and “delic,” or “delos” means “manifested.” So, in reality it simply means “mind manifested.” From the research to date, it seems the psychedelic experience is about muting the ego and bringing the mind into an observable space. In the typical adult brain, the ability to observe our thoughts in the present moment without ownership, judgement, and reaction is largely limited and dictated by how we have coped with and internalized past experiences. For many of us, our past experiences include profoundly traumatic events that are either specific in nature or that have persisted over decades.
How They Can Benefit
It is very often the ego that enforces destructive narratives. It seems that psychedelics offer an opportunity to shut the ego down for a period of time, giving the space to recognize that there is an alternative ground on which to stand, that you are in fact not identical to your ego. When the ego is no longer the most important thing, what does that look like? The ego is defensive by nature so when you take down those walls in the psyche you merge with something else. There is less of a distinction between you and the other, whether that “other” is other people in your life, the natural world, or even the universe. As these doors of the world begin to open, deep “connection” and “flow” become possible. And while it sounds trite, what seems to flow through those connections is love--incredible feelings of love and reconnection.
What WHOOP Data Shows
We learned that many of the veteran SEALs on the platform were going through these treatments. We had the opportunity to dig into the data of a few veterans, two highlighted here, who underwent psychedelic experiences (ayahuasca and psilocybin). In conversations with these individuals it is clear that there is a belief that the insight they gleaned is not a subjective opinion or idea, but rather a discovered truth. It is actual knowledge. The data outlined below suggests that the new knowledge garnered from this temporary experience had remarkable authority over the mind that influenced their physiological underpinnings. The fact that this one event can cause a reset of the mind, that a single experience could have that effect and manifest so profoundly in one's physiology, is astounding and supports much of the research that is coming out recently.
SUBJECT 1
Below are changes in WHOOP data averages for the month following post-psychedelic intervention compared to a 1-month pre-intervention baseline. Among other things, you'll see an increase in heart rate variability (HRV) and percentage of time spent in rem sleep, as well as a decrease in resting heart rate.

SUBJECT 2
Over the same time frame, Subject 2 showed an improvement in HRV, better WHOOP recoveries, and more sleep.
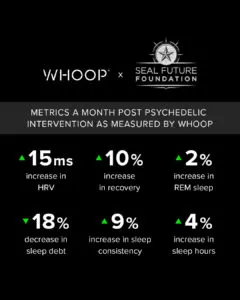
In our veteran SEAL population, we see high levels of chronic sympathetic activation (resulting in suppressed HRV) consistent with symptoms of PTSD. This over-activation results in low heart rate variability. The sustained increase observed in this data of more than 10ms over the course of a month post treatment is clinically significant. Additionally, the positive changes in sleep architecture and sleep consistency are also incredibly encouraging. It appears that the shift in perspective and mindset creates a shift in behavior, which in turn produces profound improvements in physiologic markers. The anecdotal insights around quality of life, satisfaction and clarity are profound as well. They are dramatic improvements that correlate with the data. Subject 2 (who did 5 deployments in a 7-year span) described his thoughts, actions and emotions as being perfectly harmonized without any friction or tension. While these are just two case studies, we are excited to be a part of future research with Imperial College of London to better understand how various guided psychedelic therapeutic interventions can be used to help treat PTSD as well as other mental health disorders.