Topics
- Article
- Sleep
The Optimal Sleep Playbook: Managing Sleep Debt with WHOOP
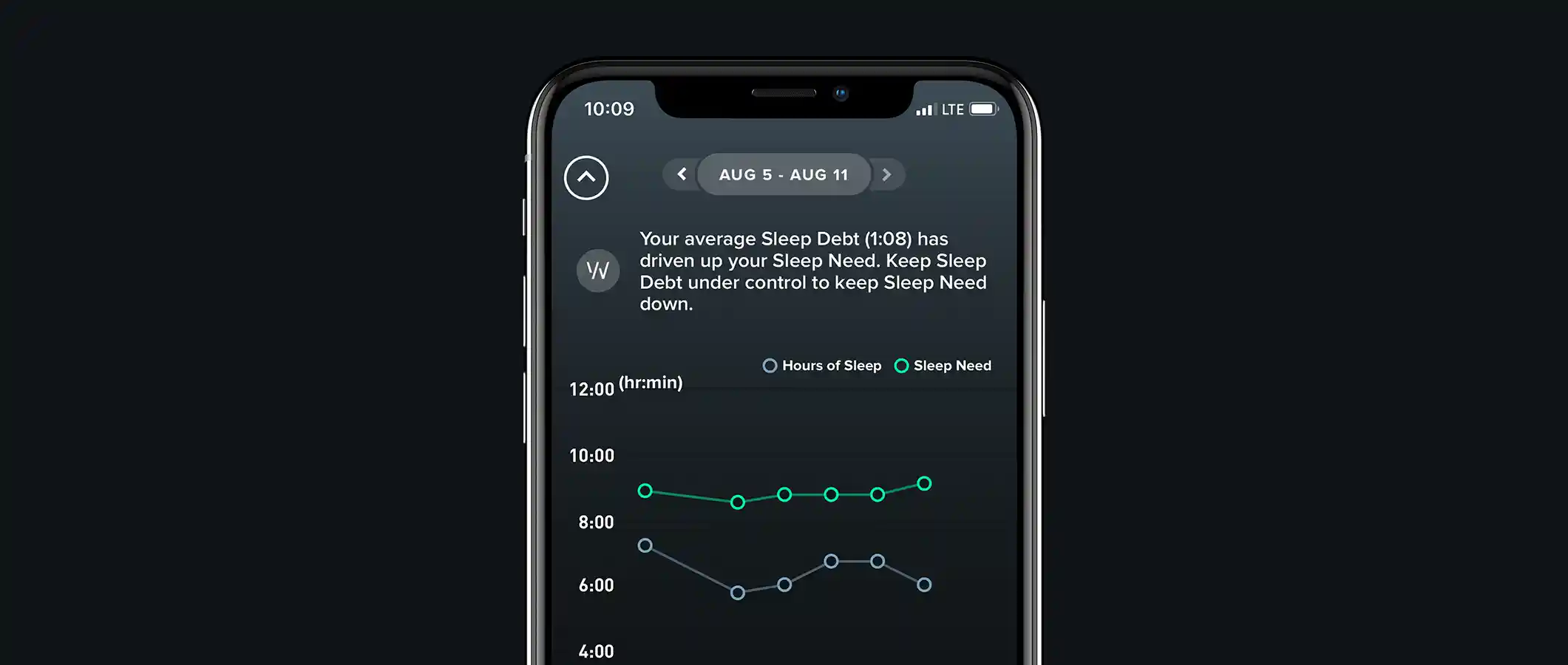
Sleep affects almost every type of tissue and system in the body, from the brain, heart and lungs, to metabolism, immune function, mood and disease resistance.
Sleep is the Trojan Horse of health! It affects almost every type of tissue and system in the body, from the brain, heart and lungs, to metabolism, immune function, mood and disease resistance. Research shows that any combination of insufficient sleep, irregular sleeping patterns or poor quality sleep increases the risk of disorders including high blood pressure, cardiovascular disease, diabetes, depression and obesity. Additionally, sleep impacts our mood, capacity to access a growth mindset, vision, agility, endurance, strength and speed. The list goes on and on, but you get the point. While sleep is a complex and dynamic process, there are behaviors I adopt that are within my control to influence outcomes related to sleep regularity, sufficiency and quality, as well as data points inside WHOOP I can leverage to better understand how my behaviors work for me (or against me). This lets me hone in on my “sleep sweet spot” and avoid a common dilemma so many of us deal with on a regular basis--racking up sleep debt.
What is Sleep Debt?
When you fail to get all the sleep your body needs at night, you begin to accumulate sleep debt. Tracked by WHOOP, sleep debt is the amount of extra sleep you need tonight because of insufficient sleep on previous nights. Below, I outline exactly how I use several features within the WHOOP app to help prevent sleep debt and maximize the overall quality of my sleep.
My Playbook for Optimal Sleep:
USE THE SLEEP Planner
I set the WHOOP Sleep Planner “peak” and pay attention to the notification each evening that tells me precisely when to go to bed and when to wake up in order to fully restore. My sleep need takes into account my recent history, strain I built that day, naps I may have taken, and any accrued sleep debt.
FOLLOW SLEEP PERFORMANCE METRICS
I use the app’s sleep performance data to ensure my sleep need and actual sleep map as close together as possible. Spending the correct amount of time in bed (not too much and not too little) gives me the best chance to optimize restorative sleep (REM and deep sleep).

MAINTAIN SLEEP CONSISTENCY
Circadian rhythms direct a wide variety of functions, including when you feel sleepy and your tendency to wake up at a certain time in the morning. In order to best hit my sleep need I must be in tune with my innate rhythm (when my body instinctively wants to sleep), so I give in to that natural preference to fall asleep as often as I can. Maintaining sleep consistency (going to bed and getting up at similar times each day) improves the efficiency of your sleep and enables you to better find your natural preference for sleep.
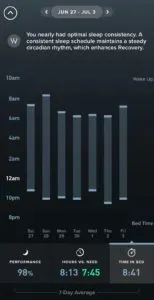
Behaviors I engage in to support this include not consuming caffeine after 1 pm, avoiding artificial lights leading into bedtime, finishing eating by 7 pm and paying close attention to when my body feels sleepy. I set up my bedtime routine so the lights are out when my peak sleep pressure hits (for me usually around 10 pm), and I always try to stay within this range of peak sleepiness by + or - 30 minutes.
MANAGE SLEEP DEBT
I strive to keep my sleep debt at zero. If I ever miss my sleep need, the following day I combat this with deep meditation, a nap, or by extending my sleep slightly that night (the Sleep Planner will automatically recommend this for you). There is also a linear relationship between athlete injury and sleep debt, which adds to the importance of keeping your debt in check.

Additionally, reducing/eliminating sleep debt allows me to achieve sleep consistency more regularly, which improves deep sleep (also known as slow wave sleep, or SWS) and REM sleep. I know that extending my sleep beyond one hour of my regular bed or wake times will impact my time spent in REM and SWS, another reason I’m careful to stay inside my most favorable sleep-wake window.
MONITOR TIME AWAKE DURING SLEEP
I click on “hours of sleep” to see how much time I’m spending in all stages of sleep. If my time awake is 30 minutes or more, I know that my daytime behaviors were off (potentially things like lack of sunlight in the am, negative stress accumulation, food or alcohol close bed, etc.) and/or my sleep environment was suboptimal (maybe not cold, quiet or dark enough).
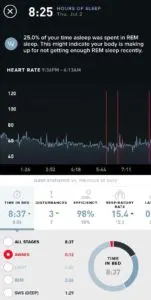
This knowledge of time awake motivates me to get back on track and ensure I am practicing daytime and pre-bed behaviors that will benefit my sleep and boost next-day recovery. In my journey to optimize sleep, I’ve come to learn and appreciate the critical contribution that it makes towards every system and process in my body. When I am in my ideal sleep groove, the mental, physical, emotional, and spiritual states necessary to truly thrive become more obvious and accessible. It is my view that sleep is not simply the third member of the “health trinity,” but rather the platform upon which other health improvements across physical exercise and nutrition are made possible.
REFERENCES
Centers for Disease Control and Prevention (CDC). Behavioral Risk Factor Surveillance System Survey Questionnaire. Atlanta, Georgia: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, 2019. Finkelstein E, Khavjou O, Thompson H, Trogdon J, Pan L, Sherry B, Dietz W. Obesity and severe obesity forecasts through 2030. American Journal of Preventive Medicine. 2012; 42(6), pp. 563-570. Lin J, Thompson T, Cheng Y, Zhuo X, Zhang P, Gregg E, Rolka D. Projection of the future diabetes burden in the United States through 2060. Population Health Metrics. 2018. Volume 16. Nyce S. Boosting employee wellness without breaking the bank. New York, New York:Towers Watson ; 2010 July. Middleton K, Anton S, Perri M. Long-Term Adherence to Health Behavior Change. American Journal of Lifestyle Medicine. 2013; 7(6): 395-404. Tomiyama AJ, Ahlstrom B, Mann T. Long-term effects of dieting: Is weight loss related to health? Social and Personality Psychology Compass. 2013; 7(12): 861-877. Loewenstein L, Asch A, Volpp K. Behavioral Economics Holds Potential to Deliver Better Results for Patients, Insurers, And Employers. Health Affairs. Vol 32, no 7.